When federal healthcare policy shifts suddenly, the impact can ripple through clinics, care providers, patients, and families alike. Recently, the Centers for Medicare & Medicaid Services (CMS) stepped in to halt a set of coverage changes that had been months in the making. For providers and patients who rely on wound care, the decision created a mix of relief as well as questions about what’s next.
On December 24, 2025, CMS announced that Medicare Administrative Contractors would withdraw the Final Local Coverage Determinations tied to skin substitute grafts and cellular- and tissue-based products. These policies were set to take effect on January 1, 2026, yet they were pulled before implementation. CMS outlined the decision in an official fact sheet, which can be reviewed directly on the CMS website.
For patients with complex or chronic wounds, this move preserved access to certain therapies that are often critical to healing.
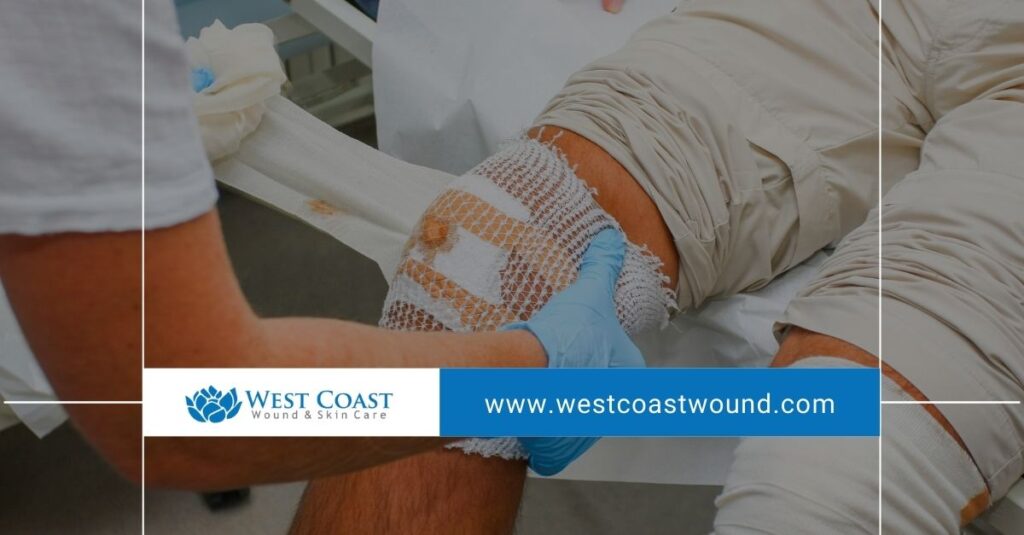
The Final LCDs in question would have significantly altered coverage criteria for skin substitute grafts and related products under Medicare Part B. By withdrawing them before January 1, CMS prevented immediate changes that could have restricted or delayed care.
Had the LCDs taken effect, providers would have faced new documentation thresholds and narrower indications for certain treatments. While oversight and evidence-based criteria are essential, abrupt changes can disrupt established care plans.
Potential impacts would have included:
The withdrawal created a pause rather than a permanent resolution, but it avoided sudden disruption as the new year began.
CMS stated that it would continue reviewing the policies and stakeholder feedback before moving forward. This potentially signals recognition of the complexity involved in caring for patients with non-healing or high-risk wounds.
National medical associations, clinicians, and patient advocates had raised concerns about access, consistency across regions, and unintended consequences.
It is important to note that the withdrawal does not mean the topic is closed. CMS may revisit revised LCDs in the future. For now, however, existing coverage frameworks remain in place, allowing providers to continue offering therapies that align with current standards of care.
For our team, this reinforces the need to stay proactive rather than reactive, keeping our patients informed while monitoring regulatory developments closely.
The withdrawal of the LCDs means that patients already receiving certain skin substitute therapies do not face abrupt changes at the start of 2026. Continuity matters, especially when healing depends on a sequence of treatments rather than a single intervention.
Patients and caregivers benefit from:
This stability supports both physical healing and emotional well-being.
At West Coast Wound & Skin Care, we help our clients navigate the healthcare landscape as part of our commitment to comprehensive care. Regulatory shifts are not just policy issues; they affect scheduling, documentation, and coordination across care settings.
Our approach centers on clear communication and adaptability. When coverage rules evolve, we work within current guidelines while preparing for possible updates.
Our support includes:
Our wound care specialist team collaborates closely with referring providers and caregivers to reduce confusion and maintain momentum toward healing.
Skin substitutes and related products are often used when standard treatments alone are not sufficient. They can help stimulate tissue regeneration, protect the wound environment, and promote closure when healing has stalled.
Each wound is different, and treatment decisions should reflect that reality. The recent CMS action underscores the need for policies that balance clinical evidence with real-world patient needs.
In our advanced wound care centers, we evaluate each case individually, considering factors such as wound type, patient health status, and response to prior treatments. This measured approach supports effective care while respecting payer requirements.
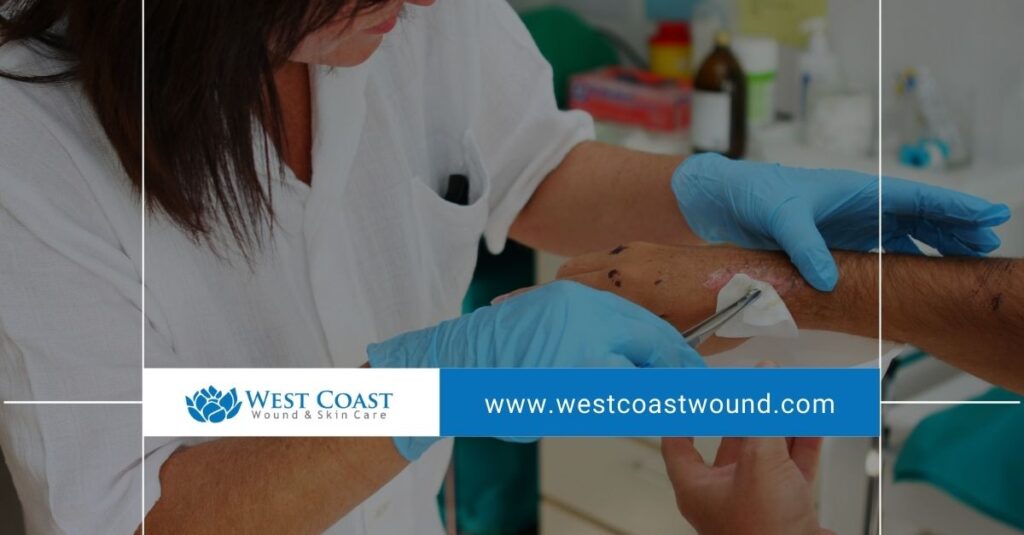
One of the strengths of our services is flexibility. We offer mobile wound care services for patients who cannot easily travel, alongside clinic locations in specific regions for those who benefit from in-person visits.
By combining mobile and clinic-based models, we reduce barriers to care and help ensure consistency, regardless of setting.
Benefits of this approach include:
This integrated model remains especially valuable as coverage discussions continue at the national level.
For individuals managing chronic or complex wounds, policy news can add another layer of stress. While CMS reviews next steps, there are practical actions patients and families can take.
You can’t control everything. But, there are actions you can take. For example, staying engaged and informed can make a meaningful difference. Beyond that, we encourage patients to:
Family members and caregivers play a key role by helping with daily care, transportation when needed, and communication with care teams.
Our services extend beyond direct wound treatment. We recognize that skin health, circulation, nutrition, and overall wellness all influence healing outcomes.
Within our scope of services, we incorporate dermatology care when skin conditions affect healing and support holistic wound care strategies that address the whole person rather than just the wound.
This integrated perspective allows us to adapt as policies evolve while staying focused on patient-centered outcomes.
The CMS withdrawal highlights how quickly the regulatory environment can change. For providers, patients, and families, preparation and communication are essential.
We continue to monitor CMS updates and trusted clinical guidance so we can respond promptly if revised LCDs emerge. By doing so, we aim to protect access, minimize disruption, and maintain high standards across all wound care services we provide.
As CMS evaluates its next steps, the current pause offers breathing room for everyone involved. It allows providers to keep delivering evidence-based treatments and gives patients confidence that their care plans remain intact for now.
For those in need of wound care, this moment reinforces the value of partnering with a care team that stays informed, adaptable, and focused on long-term healing. Our role is to guide you through both clinical and coverage complexities, ensuring that care decisions remain centered on your health and quality of life.
Many patients living with wounds reach a point where traditional therapies no longer prove beneficial. In these circumstances, chronic wound care solutions, like amniotic grafts, offer renewed potential when other methods fall short.
These grafts are biological materials that help stimulate repair in ways standard treatments cannot. As a provider of comprehensive care both in clinics and through home-based services, we see how these grafts can transform healing trajectories for people who have struggled for months or even years.
Our wound care specialist team works with individuals facing a wide range of challenges, offering tailored care in environments that best support their comfort and healing.
Many patients begin their chronic wound care with conventional approaches such as dressings, debridement, topical therapies, compression, or pressure redistribution.
These interventions are critical early steps, but some wounds resist progress due to reduced circulation, repeated trauma, infection risks, or underlying medical conditions.
Long-term wounds develop a dysfunctional environment that no longer supports healthy tissue formation. Factors contributing to stalled progression include:
• Persistent inflammation
• Accumulated biofilm
• Poor perfusion
• Cellular exhaustion within the wound bed
• Recurring pressure or friction
• Systemic conditions that limit healing capacity
When progression stops or reverses, clinicians look for solutions that stimulate new cellular activity and foster a healthier wound environment. This is where biologic grafts can become particularly effective.
Amniotic grafts, as explained by this article in the National Library of Medicine, are derived from placental tissues donated after healthy births. These tissues contain growth factors, extracellular matrix components, and anti-inflammatory properties that create an ideal foundation for new tissue formation.
Because they are naturally rich in elements that support repair, amniotic grafts offer a regenerative response many stalled wounds cannot achieve through standard therapies alone.
The attributes that make amniotic tissue valuable for chronic wound care include:
• A structure that supports cellular attachment
• Growth factors that stimulate regeneration
• Anti-scarring properties
• Anti-inflammatory benefits
• Protection through a natural biological barrier
These grafts do not replace a patient’s own tissue—they encourage the body to restart its healing cycle. For individuals who have not seen progress with standard care, this regeneration boost helps break the cycle of stagnation.
People living with diabetes experience impaired wound healing for several reasons, including neuropathy, circulation problems, and chronic inflammation.
Diabetic ulcers can benefit from amniotic grafts because the tissue adds biological activity that the body may no longer produce effectively on its own. Amniotic applications:
• Promote granulation tissue
• Help reduce inflammation
• Support better epithelial growth
• Reduce microbial presence through natural protective components
Biologic grafts can significantly accelerate closure rates in diabetic ulcers compared to standard treatments.
Venous insufficiency contributes to some of the most persistent wounds we treat. Swelling, valve dysfunction, and poor venous return create conditions that lead to repeated skin breakdown.
Compression therapy addresses the underlying cause, but some ulcers fail to progress even with proper compression.
Amniotic tissue provides benefits that complement compression therapy. Its regenerative properties support the wound at a cellular level, helping counteract chronic inflammation caused by venous disease. Patients who use both modalities together often report:
• Faster closure rates
• Reduced drainage
• Less discomfort
• Improved long-term stability
Because venous ulcers frequently recur, the regenerative foundation created by amniotic grafts supports more durable, lasting healing.
Pressure injuries arise when the skin and underlying tissues are compressed for long periods. These wounds commonly affect individuals with limited mobility or chronic illness. Healing is challenging because pressure-related damage often penetrates deep into tissue layers.
Pressure injuries benefit from amniotic grafts because:
• Growth factors help stimulate new tissue formation
• Anti-inflammatory effects reduce secondary tissue breakdown
• Structural proteins strengthen the wound platform
• The graft provides a protective barrier during early healing
For patients who rely on in-home visits or clinic appointments for chronic wound care, biologic support can reduce complications that are common with deep tissue injuries.
Not every wound requires a biologic graft, but when a patient’s wound has stalled or shows signs of chronicity, we evaluate whether grafts may improve outcomes. Our clinicians assess wound depth, location, tissue behavior, circulation, infection risk, and health history before considering graft use.
Our advanced wound care centers provide structured environments for graft placement, while our mobile services allow appropriate grafts to be applied directly in the home when medically suitable.
When graft therapy is recommended, our approach may include:
• Thorough wound bed preparation to remove barriers to healing
• Stabilization of inflammation and drainage levels
• Application of the graft in a clean, controlled environment
• Protective dressing layers to maintain an optimal healing environment
• Ongoing follow-up through clinic visits or in-home services
We also provide guidance to help patients and caregivers maintain the conditions that support long-term healing.
Skin conditions such as eczema, infections, or chronic irritation can worsen wound environments. By offering dermatology care as part of our services, we help address contributing factors that may slow healing or increase the risk of new wounds forming.
Managing surrounding skin effectively makes graft applications more successful and supports overall recovery.
Our goal is to approach each patient’s case from multiple angles to ensure that the wound—and the skin around it—improves consistently.
When we evaluate a patient for graft therapy, we look beyond the visible wound. Each patient’s nutrition, mobility, circulation, chronic conditions, and lifestyle contribute to wound behavior. A targeted biologic graft alone may not be effective unless the patient’s broader needs are addressed.
Through holistic wound care, we can take into account:
• Pressure relief strategies
• Edema management
• Nutritional support coordinated with medical providers
• Mobility limitations and daily routines
• Environmental factors that influence healing
Treating the whole patient helps ensure that patients are treated with biologic grafts within an optimized healing environment.
Some patients struggle to travel due to mobility limitations, medical conditions, or transportation issues. In those situations, our mobile services allow us to bring high-level care directly to the home. While not every graft type is suitable for home application, some can be safely placed during in-home visits.
This approach enhances continuity for patients who otherwise might experience delays or gaps in treatment. Our clinicians bring the necessary equipment, provide education, and maintain consistent monitoring, ensuring that healing remains on track.
For patients facing long-standing wounds, specialized biologic solutions play a vital role in improving outcomes. By bringing together advanced therapies, clinic-based care, in-home services, and comprehensive support, we help individuals recover with greater stability and confidence.
Our chronic wound care services are designed to ensure patients receive the care they need, providing a clearer path forward.
At West Coast Wound Care, we are thrilled to share that we’ve recently launched wound treatment in the Boston area, bringing our full suite of wound healing services to New England. We now serve patients not only through our clinics but also via mobile options.
As a result, we can bring cutting-edge wound healing technology, evidence-based medicine, and compassionate care to more people. With multiple options on hand, we believe in making wound treatment as accessible as possible.
Since establishing operations in Boston, we have set up wound care clinics serving greater Boston, including both downtown and suburban locations. In addition to clinic-based settings, our mobile wound care capabilities now extend into Boston neighborhoods, hospitals, long-term care facilities, and patients’ homes.
Our goal is to ensure that those with limited ability to travel still receive top-quality treatment from a wound care specialist, tailored to their individual situations.
Following this launch, we are looking ahead to expanding further into neighboring New England states. We intend to grow our footprint into Massachusetts’ outer regions in addition to New Hampshire, Vermont, Maine, Connecticut, and Rhode Island.
Our strategy includes forging partnerships with local clinics, healthcare systems, and home care providers to bring our model of care to more communities.
At West Coast Wound Care, our services cover the full spectrum of modern wound healing so that patients at every stage of recovery can find care that matches their needs. Every wound is different, and we offer a personalized plan designed to promote faster healing, reduce pain, and restore function.
We provide advanced diagnostic evaluations, which means that our clinicians don’t just look at the wound itself but also at the underlying causes. This can involve vascular assessments, laboratory tests, and imaging to better understand circulation, infection risk, and other factors slowing down healing. Because many wounds stem from conditions such as diabetes, venous disease, or immobility, our diagnostic approach helps us treat the whole patient rather than just the wound.
Our surgical debridement services are performed by highly trained providers who carefully remove non-viable or infected tissue. This process reduces bacteria, decreases inflammation, and creates a healthy environment for new tissue growth. In our clinics, we can do this with precision instruments and local anesthetics to minimize discomfort, while our mobile teams bring the same level of expertise directly to the bedside.
When wounds are especially large or resistant to healing, we offer skin grafting procedures. This may include autografts (from the patient’s own skin) or biologic dressings that provide a scaffold for new tissue growth. Our specialists match the graft type to the wound’s specific needs and monitor its integration closely.
We also specialize in wound vacuum therapy (negative pressure wound therapy). This advanced treatment involves placing a sealed dressing over the wound and applying gentle suction. It helps remove excess fluid, improves blood flow, and encourages tissue granulation, dramatically speeding up healing times for certain types of wounds.
Compression therapy is another cornerstone of our practice. For patients with venous insufficiency or chronic swelling, compression bandages or garments can be critical to controlling edema and improving circulation. We not only apply these treatments but educate patients and caregivers on their proper use, which is essential for success.
Our team also performs biopsies when a wound appears atypical or does not respond to standard treatments. This allows us to rule out underlying conditions such as malignancy, vasculitis, or rare infections and adjust care accordingly.
Finally, our telemedicine support and virtual follow-ups extend our care beyond clinic walls. Patients recovering at home can send images, update our clinicians on progress, and receive prompt guidance, reducing the need for travel and ensuring continuity of care.
We are more than a group of clinicians; we are a coordinated team of physicians, nurses, and allied health professionals who share a passion for helping people heal. Every member of our staff has specialized training in wound assessment and advanced interventions. This ensures that whether you come into one of our clinics or receive care at home, you’re getting the same high standard of expertise.
Our approach begins with listening. We take time to understand not only the wound itself but also your medical history, daily activities, support systems, and goals. From there, we create an individualized care plan that fits your life. For instance, a patient with a diabetic foot ulcer who lives alone may need more frequent visits and education about self-care, while someone recovering from surgery might need intensive therapy initially and then transition to virtual check-ins.
We coordinate closely with primary care providers, surgeons, podiatrists, and home health nurses. By sharing records and updates, we reduce duplication of efforts and ensure that everyone involved in your care is on the same page. This team-based model lowers complication rates and improves patient satisfaction.
Prevention is also central to how we care. We work with patients to identify risk factors for recurrence — from footwear choices to nutritional deficiencies to mobility challenges — and develop strategies to keep wounds from coming back. Our staff educates patients and caregivers on dressing changes, offloading, and lifestyle adjustments to give healing the best possible chance.
Because navigating insurance can be daunting, our administrative team helps patients understand their coverage and out-of-pocket costs before treatment starts. We accept Medicare and many other plans, which makes our services accessible to a broad range of patients in the New England region.
When you select West Coast Wound Care for your wound healing needs, you’re choosing a partner that combines convenience, expertise, and compassion. The benefits of working with us go beyond the procedures themselves:
In New England specifically, our expansion means patients no longer have to wait for a referral to a distant wound center. By opening clinics and deploying mobile teams across Massachusetts and beyond, we’re reducing wait times and making specialized care available closer to home.
This local presence also allows us to develop relationships with area hospitals, rehabilitation centers, and home health agencies, streamlining the patient experience even further.
As we look to expand beyond Boston, we are exploring service area growth in:
Each new region will be accompanied by clinic locations and mobile service offerings, allowing us to adapt to the needs of urban, suburban, and rural populations alike.
When you need wound treatment from experts who combine clinic-based care with bedside solutions, West Coast Wound Care is here to serve. If you’re in Boston or surrounding New England states, please contact us today to make an appointment.